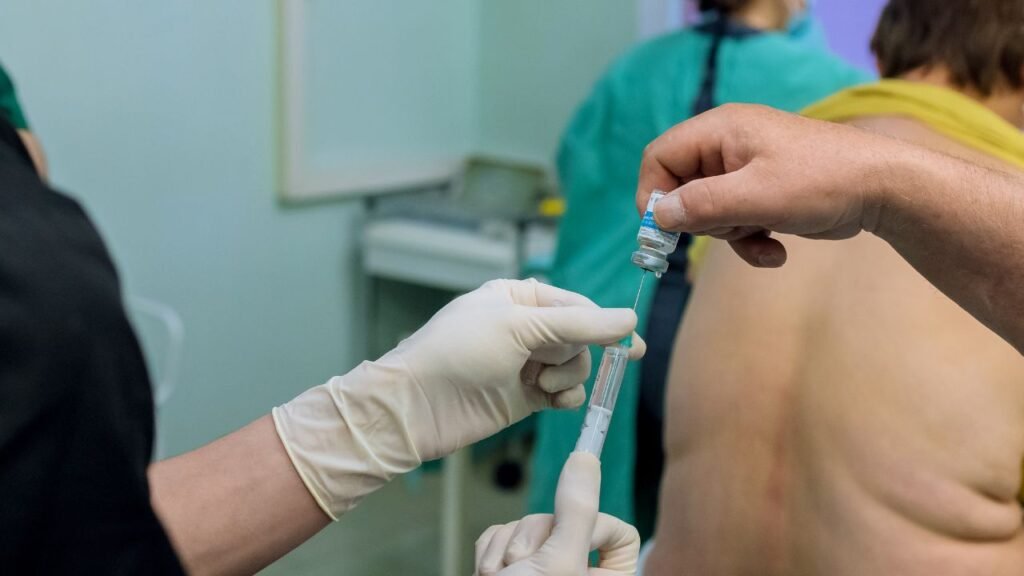
Epidural steroid injections are among the most common interventional procedures for nerve-related back and neck pain. If you’re experiencing sciatica, herniated disc pain, or spinal stenosis, your physician may have recommended this treatment. While epidural steroid injections can provide temporary relief by reducing inflammation around compressed nerve roots, understanding what to expect from the procedure itself, potential side effects, and long-term limitations helps you make informed decisions about your pain management strategy.
This comprehensive guide explains how epidural steroid injections work, who benefits most from them, and why they’re considered a short-term solution rather than a permanent fix for structural spinal problems.
Key Takeaways
- Temporary symptom relief, not structural healing: Injections reduce inflammation for 6-12 weeks on average, but don’t repair herniated discs, bone spurs, or stenosis. Pain typically returns when medication wears off.
- Common side effects resolve quickly: Flushing (20-30%), blood sugar elevation in diabetics (10-20%), and insomnia (10-15%) typically resolve within 24-48 hours; serious complications like infection occur in less than 1% of cases.
- Limited to 3-4 injections per year maximum: Effectiveness diminishes with repeated use due to cumulative risks, including tissue weakening, bone density loss, and adrenal suppression.
- Best used as a bridge to rehabilitation: Ideal for patients with confirmed nerve compression who haven’t responded to 6-12 weeks of conservative treatment and need temporary relief to participate in physical therapy.
- Multiple alternatives offer long-term solutions: Physical therapy addresses underlying deficits, regenerative medicine may support natural healing, and surgery remains an option for progressive neurological symptoms or failed conservative care.
What Is An Epidural Steroid Injection?
An epidural steroid injection places corticosteroid medication into the epidural space, the area containing fat and veins surrounding the dura mater (protective membrane around your spinal cord).
Anatomy & Components:
- Epidural space contains fat and veins surrounding the dura mater
- Two primary injection approaches available:
- Interlaminar approach: Needle inserted between vertebrae (laminae)
- Transforaminal approach: Needle inserted through neural foramen (opening where nerve roots exit)
- Corticosteroid medication bathes nerve roots within the epidural space
How Do Epidural Steroid Injections Relieve Pain?
Epidural steroid injections reduce inflammation around compressed or irritated nerve roots, providing targeted relief at the source of your pain.
Mechanism of Action:
- Corticosteroid reduces inflammation around compressed or irritated nerve roots
- Anti-inflammatory medication delivered directly to pain source via epidural space
- Reduces swelling around nerve structures
- Decreases pain signal transmission from affected nerves
What Conditions Are Typically Treated With Epidural Steroid Injections?
Epidural steroid injections address nerve-related pain conditions caused by compression or inflammation.
Common Conditions Treated:
- Sciatica (radiating leg pain from nerve compression)
- Herniated discs (bulging or ruptured spinal discs)
- Spinal stenosis (narrowing of spinal canal)
- Radiculopathy (nerve root inflammation causing arm or leg pain)
- Degenerative disc disease (age-related disc breakdown)
- Foraminal stenosis (narrowing of nerve exit pathways)
- Post-laminectomy syndrome (persistent pain after spinal surgery)
What To Expect Before, During, And After An Epidural Steroid Injection?
The epidural steroid injection procedure follows strict protocols to ensure safety and effectiveness. From pre-procedure preparation through post-injection recovery, understanding each phase helps you know what to expect and how to optimize your results, giving you clear procedure expectations before your appointment.
What Should You Do To Prepare For An Epidural Steroid Injection?
Proper preparation ensures your procedure goes smoothly and minimizes complications.
Pre-Procedure Preparation Steps:
- Fasting or stopping food intake for a certain period (if required by facility)
- Discontinuing blood thinners (under doctor’s advice, typically 3-7 days prior)
- Bringing a friend or family member to drive after the procedure
- Informing the doctor of allergies or pre-existing conditions (especially diabetes, bleeding disorders, active infections)
- Arranging time off work for procedure day and potential recovery period
- Wearing comfortable, loose-fitting clothing to appointment
What Happens During The Procedure?
Epidural steroid injections require precision and advanced imaging for safe, effective delivery.
Step-by-Step Procedural Details:
- Fluoroscopy (live X-ray) guidance is mandatory for accurate needle placement and patient safety
- Patient positioned prone (face down) or lateral (side-lying) on procedure table
- Local anesthetic is applied to injection site to numb skin
- Tuohy needle inserted using loss-of-resistance technique to locate epidural space
- Contrast dye injected first to confirm proper needle placement and rule out vascular (blood vessel) penetration
- Corticosteroid medication injected: typically triamcinolone or betamethasone at doses of 40-80mg
- Strict sterile technique maintained throughout to minimize infection risk
How Long Does An Epidural Steroid Injection Take?
Procedure Duration:
- Total procedure time: 15-20 minutes
- Most time spent on precise needle positioning using fluoroscopy
- Actual medication injection takes only seconds once needle properly positioned
What Happens After The Injection?
Following your injection, specific recovery guidelines help optimize results and minimize complications.
Post-Procedure Instructions and Timeline:
- Activity restrictions for 24 hours following the procedure
- Resting recommended for first 24-48 hours to allow medication to settle
- Avoiding strenuous activities for 24-48 hours
- Possible localized post-injection soreness at injection site (usually subsides within hours)
- Possible temporary flushing sensation (warmth and facial redness)
- Monitoring for any unusual reactions or side effects (numbness, severe headache, fever)
- Following up with doctor if pain worsens or new symptoms develop
- Resuming normal activities gradually as tolerated after 24-hour restriction period
How Quickly Will You Feel Relief After An Epidural Steroid Injection?
Pain relief develops gradually as inflammation subsides around compressed nerve roots.
Pain Relief Timeline:
- Initial relief begins: 2-7 days after injection (corticosteroid onset time)
- Peak pain relief occurs: 1-2 weeks post-injection (when anti-inflammatory effect is strongest)
- Local anesthetic (if used) provides immediate but very brief relief (1-4 hours)
- Full therapeutic effect develops gradually as inflammation subsides over first 1-2 weeks
What Are The Side Effects Of Epidural Steroid Injections?
Like all medical procedures, epidural steroid injections carry potential side effects ranging from common, minor reactions to rare but serious complications. Most side effects are temporary and resolve within days, but understanding both common and serious risks helps you make informed decisions and recognize when to seek medical attention.
What Are The Most Common Side Effects?
Most patients experience mild, temporary side effects that resolve without intervention.
Common Side Effects with Incidence Rates:
- Flushing (facial warmth and redness): 20-30% of patients, typically resolves within 24-48 hours
- Blood sugar elevation in diabetics: 10-20% of diabetic patients require careful monitoring for several days
- Insomnia (sleep disturbance): 10-15% of patients, usually transient and resolves within days
- Soreness at injection site: Common, usually mild, subsides within hours to 1-2 days
- Mild headaches: Often related to anxiety or vasovagal response, temporary
- Temporary increase in pain (initial flare): Can occur as medication settles, typically resolves within 24-48 hours
- Nausea: Generally mild and transient
- Dizziness or lightheadedness: Usually brief, related to stress response or position changes
What Are The Rare Or Serious Side Effects?
While uncommon, serious complications require immediate medical attention if they occur.
Rare but Serious Complications with Incidence Rates:
Dural puncture headache (PDPH): 1-2% incidence
- Occurs when needle inadvertently punctures dura mater, causing cerebrospinal fluid (CSF) leakage
- Characterized by severe headache worse when upright, relieved by lying down
- May require blood patch procedure if persistent
Infection: Less than 1% (<1%) incidence
- Potential infections: epidural abscess, meningitis, osteomyelitis, or soft tissue abscess
- Prevented through strict sterile technique
Bleeding or hematoma formation: Rare
- Risk increased with blood thinners
- Can potentially compress nerve structures if significant
Nerve damage: Very rare with fluoroscopic guidance
- Direct trauma to nerve root can cause pain, numbness, or weakness
Allergic reactions: Rare
- Reactions to corticosteroid, local anesthetic, or contrast dye
- Can range from mild skin reactions to severe anaphylaxis
How Long Do The Side Effects Last?
Most side effects are temporary, resolving within hours to days.
Side Effect Duration by Type:
- Flushing: Resolves within 24-48 hours in most cases
- Insomnia: Transient, typically resolves within 2-5 days
- Blood sugar changes in diabetics: May require monitoring for 3-7 days post-injection
- Post-injection soreness: Usually lasts hours to 1-2 days
- Headaches (non-PDPH): Typically resolve within 24-48 hours
- Most common side effects: Temporary, lasting hours to a few days maximum
- Dural puncture headache: Can persist 3-7 days if untreated; resolves within 24-48 hours with blood patch
Are There Long-Term Risks With Epidural Steroid Injections?
Repeated use carries cumulative risks that limit how frequently these injections can be safely administered.
Long-Term Concerns with Repeated Use:
- Diminishing effectiveness: Returns decrease with repeated use, particularly after 3-4 injections per year
- Tissue weakening: Repeated corticosteroid exposure can weaken ligaments and connective tissues over time
- Bone density reduction: Prolonged steroid exposure may contribute to osteoporosis (bone thinning)
- Adrenal suppression: Repeated injections can temporarily suppress body’s natural cortisol production
- Masking progressive problems: Symptom relief can delay diagnosis and treatment of worsening structural damage
- Not regenerative: Does not heal or repair underlying structural damage (herniated discs, bone spurs, stenosis)
Why Are Epidural Steroid Injections Considered A Short-Term Solution?
Epidural steroid injections provide temporary symptom relief but do not address the underlying structural problems causing your pain. Understanding these fundamental limitations helps you evaluate whether this approach aligns with your long-term health goals or whether alternative treatments might offer more lasting solutions.
Why Do Epidural Steroid Injections Provide Temporary Relief?
These injections address symptoms without correcting the underlying cause of your pain.
Fundamental Limitations:
- Addresses inflammation symptoms, not underlying structural causes
- Does not repair damaged discs, bone spurs, or areas of stenosis
- Steroid medication eventually metabolizes and wears off
- Underlying mechanical compression or degeneration persists after medication effect ends
- Cannot reverse degenerative processes (arthritis, disc degeneration)
- Provides symptomatic relief while the structural problem remains unchanged
How Long Do The Effects Of An Epidural Steroid Injection Last?
Relief duration varies significantly among patients based on condition severity and individual response.
Duration of Pain Relief:
- Typical duration: 6-12 weeks for most patients
- Some patients experience relief lasting several months
- Rare cases report relief extending up to one year
- Duration varies significantly based on:
- Severity of underlying condition
- Individual patient response
- Degree of structural damage
- Pain relief is temporary, not permanent
How Often Can You Receive Epidural Steroid Injections?
Safety concerns limit how frequently you can receive these injections.
Frequency Limitations:
- Recommended maximum: 3-4 injections per year
- Spacing between injections typically 6-12 weeks minimum
- Effectiveness diminishes with repeated annual use
- More frequent injections increase risk of:
- Tissue weakening
- Bone density loss
- Adrenal suppression
- Long-term complications
What Are The Limitations Of Epidural Steroid Injections In Pain Management?
Understanding what epidural steroid injections cannot do is as important as knowing what they can accomplish.
Key Limitations:
- Temporary relief only – does not address root structural problems
- Not a regenerative therapy – does not heal or repair damaged tissue
- Can mask symptoms – potentially delaying definitive treatment when needed
- Diminishing effectiveness – returns decrease after 3-4 annual injections
- Does not prevent disease progression – underlying condition continues to worsen
- Cannot replace surgery when structural intervention is medically necessary
- Limited by corticosteroid safety profile – cannot be used indefinitely
Understanding the difference between symptom relief and long-term joint support helps you evaluate whether this short-term approach aligns with your healing goals.
Who Should Consider Epidural Steroid Injections?
Epidural steroid injections work best for specific patient profiles and conditions. Understanding whether you’re an ideal candidate, or whether contraindications make this approach unsuitable, helps you and your physician determine if this treatment aligns with your medical needs and safety profile.
What Are The Ideal Candidates For Epidural Steroid Injections?
Certain patient profiles benefit most from this intervention.
Best Candidates for ESI:
- Individuals with chronic back pain lasting more than 12 weeks
- Those who haven’t responded to conservative treatments (physical therapy, oral medications) after 6-12 weeks
- Patients with herniated discs or nerve compression confirmed by imaging (MRI or CT)
- Those experiencing significant radicular pain (nerve-related arm or leg pain) affecting mobility or quality of life
- Patients with spinal stenosis causing neurogenic claudication (leg pain with walking)
- Individuals seeking temporary relief to participate in physical therapy or rehabilitation
- Those with acute flare-ups of chronic conditions
- Patients who are not surgical candidates or wish to avoid surgery
Who Should Avoid Epidural Steroid Injections?
Certain medical conditions make this procedure unsafe or inappropriate.
Contraindications: Individuals Who Should Not Receive ESI:
- Active infections at the proposed injection site or systemic infection
- Severe allergies to steroids or local anesthetics
- Uncontrolled diabetes (blood sugar consistently above 200 mg/dL)
- Pregnancy (especially first trimester, due to unknown effects on fetus)
- Blood clotting disorders (hemophilia, severe thrombocytopenia)
- Patients taking anticoagulants (blood thinners) without medical clearance to hold medication
- Active bleeding or recent hemorrhagic stroke
- Immunosuppressed patients (higher infection risk)
- Individuals with severe osteoporosis (increased fracture risk)
How Do Underlying Conditions Affect The Effectiveness Of Epidural Steroid Injections?
Pre-existing medical conditions significantly impact both safety and treatment outcomes.
Condition-Specific Considerations:
- Diabetic patients: 10-20% experience blood sugar elevation requiring insulin adjustment and monitoring for 3-7 days
- Severe structural damage (advanced stenosis, large herniation): May experience limited or shorter duration of benefit
- Progressive nerve compression: Relief duration often shorter, may indicate need for surgical intervention
- Autoimmune conditions: May affect steroid response and inflammation control
- Obesity: May reduce effectiveness due to anatomical challenges and increased inflammatory load
- Smoking: Slows healing response and may reduce treatment effectiveness
- Prior failed ESI: Lower likelihood of success with additional injections
What Are The Alternatives To Epidural Steroid Injections For Pain Management?
Epidural steroid injections represent just one option in a comprehensive pain management approach. Multiple alternative treatments exist, ranging from conservative therapies to advanced regenerative medicine and surgical interventions. Evaluating these alternatives helps you choose the approach best suited to your condition, goals, and long-term health priorities.
What Are Non-Steroidal Pain Relief Options?
Conservative approaches offer effective relief for many patients without injection risks.
Conservative Treatment Alternatives:
- NSAIDs (ibuprofen, naproxen) for inflammation reduction
- Neuropathic pain medications: Gabapentin or pregabalin for nerve-related pain
- Acupuncture: Traditional Chinese medicine approach for pain modulation
- Chiropractic care: Spinal manipulation and mobilization
- Physical therapy (PT): Strengthening, flexibility, and postural training
- Hot or cold packs: Thermal modalities for symptom management
- Massage therapy: Soft tissue mobilization and relaxation
- Activity modification: Avoiding aggravating positions and movements
- Weight management: Reducing mechanical load on spine
- TENS units: Transcutaneous electrical nerve stimulation for pain relief
How Do Physical Therapy And Lifestyle Changes Compare To Steroid Injections?
Physical therapy and lifestyle modifications address underlying causes rather than just symptoms.
Physical Therapy Benefits:
- Timeline for improvement: 6-12 weeks for significant functional gains
- Addresses underlying muscle weakness and flexibility deficits
- Improves long-term function and movement patterns
- Lower risk profile than injections (no infection or bleeding risk)
- Teaches self-management strategies for long-term pain control
- Can prevent recurrence through strengthening and proper body mechanics
Lifestyle Modification Impact:
- Weight loss reduces mechanical stress on spine structures
- Posture correction decreases abnormal loading patterns
- Ergonomic adjustments prevent aggravation during daily activities
- Smoking cessation improves disc nutrition and healing capacity
What Surgical Options Are Available For Chronic Pain Management?
When conservative treatments fail, surgical interventions may become necessary.
Surgical Interventions:
- Decompression surgery (laminectomy): Removes bone/tissue compressing nerves
- Microdiscectomy: Removes herniated disc material pressing on nerve roots
- Spinal fusion: Stabilizes unstable vertebrae, typically for spondylolisthesis or severe instability
- Foraminotomy: Widens neural foramen to relieve nerve compression from foraminal stenosis
Surgery is typically considered after failed 6-12 months of conservative treatment, including injections.
Indications for Urgent Surgery:
- Progressive neurological weakness
- Loss of bowel/bladder control (cauda equina syndrome)
- Severe, intractable pain unresponsive to all other treatments
Emerging Alternatives:
- Platelet-Rich Plasma (PRP) therapy: Investigational status, uses concentrated healing factors from the patient’s own blood
- Stem cell therapy: Experimental regenerative approach, not FDA-approved for spinal conditions, learn more about stem cell therapy for back pain
- Minimally invasive procedures: Percutaneous disc decompression, intradiscal procedures
Are Epidural Steroid Injections Right For You?
Epidural steroid injections provide temporary inflammation reduction but do not address underlying structural damage. This fundamental limitation makes them a short-term solution rather than a long-term healing strategy. Understanding when these injections serve a useful purpose, and when alternative approaches might better serve your goals, requires careful evaluation of your condition, treatment history, and desired outcomes.
How Do You Know If An Epidural Steroid Injection Is The Right Treatment Option?
Making an informed decision requires evaluating multiple factors about your specific condition and goals.
Decision Framework:
- Consider if conservative treatments (PT, medications) have been tried for adequate duration (6-12 weeks minimum)
- Evaluate if pain is significantly affecting quality of life and daily function
- Assess whether temporary relief would allow participation in physical therapy or rehabilitation
- Determine if you’re a candidate based on medical history and absence of contraindications
- Consider if you have confirmed nerve compression on imaging (MRI or CT scan)
- Evaluate if you’re seeking a bridge to other treatments rather than standalone solution
What Questions Should You Ask Your Doctor Before Choosing An Epidural Steroid Injection?
These essential questions help you make an informed treatment decision.
Essential Questions to Discuss:
- What is causing my pain, and will an injection address the root cause or just symptoms?
- What are my expected outcomes based on my specific condition and imaging findings?
- How long will relief last, and what happens when the medication wears off?
- What are the risks specific to my health conditions (diabetes, blood thinners, autoimmune disease)?
- What alternative treatments should I consider before or alongside injections?
- How many injections will I likely need, and what is the long-term plan for my condition?
- What percentage of patients with my specific condition experience significant relief?
- Will the injection help me participate in physical therapy or other rehabilitative treatments?
- Am I a candidate for regenerative medicine alternatives that might provide longer-lasting results?
- What are the signs and symptoms that would require immediate medical attention after the procedure?
- If the injection doesn’t work, what are my next steps?
Ready to explore solutions that support healing, not just symptom management? Contact Integrated Spine, Pain & Wellness to discover regenerative medicine alternatives designed to support your body’s natural healing capacity.